The last thing Rina Risper wants in her neighborhood is another hub for recovering drug addicts.
She — along with more than 100 residents in Lansing’s Walnut Neighborhood — last month submitted a petition against a proposed, 14-bed residential treatment facility at a now-vacant office building off Pine Street. It’s too close to a nearby middle school, and addiction can often breed undesirable neighbors, she contended.
“This is not about stigma,” Risper penned in a letter to city officials. “Our neighborhood already has a 50-bed substance abuse facility that is around the corner.”
“This is about having a responsibly balanced neighborhood,” she added.
But advocates for enhanced substance abuse treatment options contended some perspectives — much like those voiced from Walnut Neighborhood residents — will need to shift if Ingham County is ever going to make significant progress in curbing the number of fatal overdoses amid a growing, nationwide opioid epidemic.
Mid-Michigan Recovery Services aims to renovate the former School for the Blind building into an expanded men’s treatment facility, but it first needs a special land use permit for the plans to come to fruition. A public hearing has yet to be held, but a growing contingency of local residents have pushed back against the idea.
Local resident Kris Reader wrote another facility “dumping on” his neighborhood would cause drug dealers to gravitate to the area and almost certainly spell an increase in criminal activity. Others claimed they were sexually harassed by patients from a nearby facility. Another man said a recovering alcoholic asked him to buy him booze.
“This is something that treatment facilities face wherever they go,” said Dani Meier, chief clinical officer for Mid-State Health Network. “It’s this ‘not-in-my-backyard’ mentality and I don’t have a solution to it by any means.”
“It’s going to be an uphill battle as long as we have these stigmas, and it’ll take some education,” Meier added.
And county residents — particularly those in Lansing who already face a market stretched thin in terms of options for addiction treatment services — can’t afford to squander an opportunity to save lives.
Meier said the addictive grip that opioids and other substances have on the community will only tighten without a change.
‘A tragic loss of life’ Opioid abuse — specifically the deadlier, synthetic varieties — for years has ravaged the nation as thousands die annually from accidental overdoses and children are ripped from homes in the wake of a growing epidemic. And a recently released report from Sparrow indicates the situation locally has gotten worse and will continue to worsen this year.
“It’s really been a tragic loss of life, and it’s growing and expanding in part because more synthetic opioids are finding their way into the market,” Meier said, noting Lansing is underserved by its three existing treatment facilities. “They’ll use whatever they can get their hands on, and often people don’t take proper precautions.”
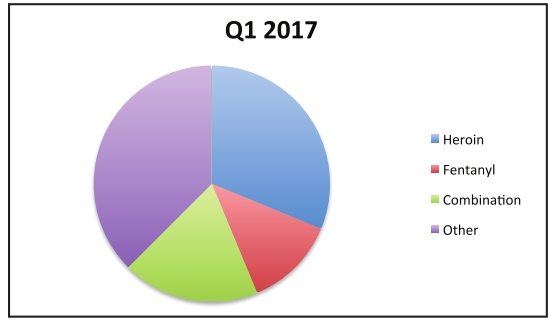
Sparrow Department of Forensic Pathology’s latest quarterly report, released Sunday evening, showed the region continues to struggle with opioid abuse as accidental, drug-related overdose deaths remain steady into the first half of the year. And Ingham County, in particular, bears the brunt of ongoing concerns.
At least 46 people there died from an accidental overdose so far this year, climbing from the number reported this time last year, according to reports provided by Sparrow. The data suggests the number of accidental and fatal overdoses — fueled largely by fentanyl — will likely outpace the number tracked over the last several years.
Countywide opioid surveillance reports further indicate 70 children this year were removed from their homes by the state Department of Health and Human Services. Forty of those cases involved substance abuse and 29 involved opioids, according to the report. Those statistics aren’t included in reports from the last two years.
But if overdoses remain consistent for the rest of the year, Ingham County might just break an all-time record.
“We’re facing an opioid epidemic, and Ingham County is no exception to that,” said County Health Officer Linda Vail. “Drug overdose deaths have now become the leading cause of accidental deaths in our country, followed only by falls and motor vehicle accidents. I don’t think there’s an immediate solution.”
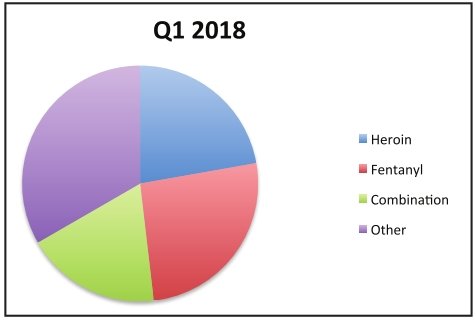
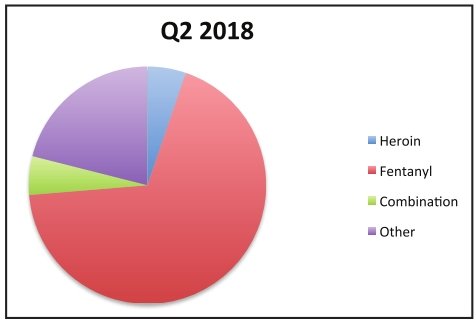
About half of this year’s accidental overdoses involved some variety of fentanyl — a dangerous and synthetic opioid prescribed only for the most severe cases of cancer-related pain. Officials said street dealers often use it to cut their heroin to elicit a more powerful high or quickly trigger a longstanding addiction for newer clientele.
They don’t want to kill their customers, but with a substance billed to be as much as 10,000 times more potent than heroin, the unintended and fatal consequences can be unavoidable, officials said. Ingham County sheriff ’s deputies won’t field-test powdery substances out of fear of an accidental overdose.
“Drugs like heroin today are not the type that was available on the streets in the ‘60s and ‘70s during their parents’ generations,” said sheriff’s Capt. Greg Harris. “It’s more potent. It’s more prevalent. Every dealer wants to be known for having the best product but it can only be so pure. That’s where fentanyl comes into play.”
‘Chasing the tail of this dragon’ Every first responder in the county now carries a naloxone kit, Harris said. The opioid-reversal medication can sometimes require two or three doses to take effect depending on the user and potency of their drugs but officials fear deadly overdoses would be far more frequent without them, particularly in the more urban areas.
Reports indicated naloxone — some times referred to by the brand name Narcan — was deployed on 373 separate occasions last year amid 281 overdose incidents. About 90 percent of those who were treated survived. And 240 of those countywide overdoses occurred within the city of Lansing alone, reports elaborate.
“Naloxone is a great rescue drug,” Vail added. “But it’s not treatment. It’s not recovery. It’s reactive.”
Ingham County Prosecutor Carol Siemens continues to levy felony drug-dealing charges against lower-level street dealers and routinely pursues possession cases against their customers. But she recognizes her jurisdiction ends at the county line and it doesn’t do much to dam the stream of drugs flooding into the country.
“Having your kids removed can be a wakeup call,” Siemens added. “Other times they’ll go to jail or they’ll nearly die from an overdose.
That can be a wake-up call too. For some people, they’re just pissed off that it ruined their high and they kind of missed the fact that their life was saved. It’s a very insidious thing.”
Harris said the fentanyl finding its way onto the streets isn’t coming from a doctor’s office nor are cancer patients selling off the last of their supplies. The opioids his deputies typically find come from online vendors and continual changes to chemical compositions can pose an obstacle to even the most stringent federal regulations.
“We’re constantly chasing the tail of this dragon,” said Harris. “The best we can do at a local level is go after the dealers who are pushing it on the street, but we recognize there are more layers above them.”
‘A lot of stigma’ Siemens suggested the simplest solution to the epidemic centers on motivating users to kick their habits before they turn deadly. Rapid response teams — comprised of certified counselors and first responders — routinely visit with residents in the immediate aftermath of an overdose to explain different options for treatment.
Good Samaritan laws largely shield those who overdose and seek medical treatment from facing criminal charges, Siemens added. Specialty courts are also geared more toward rehabilitation than punishment. But those are largely reactive measures. Proactive solutions for treatment can sometimes be few and far between, she said.
Vail said medical providers need special training and certifications before they can dole out medication for substance abuse treatment, and those requirements are keeping some physicians out of the game altogether. Ongoing misconceptions about addiction treatment also continue to pose a roadblock to progress, she said.
“We need to understand that addiction is a chronic brain disease,” Vail added. “This is is a health issue and it needs to be treated like one. We need to find recovery methods and support them.”
Advocates for years have urged local communities to expand their treatment options, but misconceptions surrounding the nature of addiction are difficult to defeat. And Vail conceded Lansing might not be ready for clean needle services or injection sites like ongoing proposals in metropolitan areas such as Seattle and San Francisco.
“There’s been a lot of effort on the prevention side to try to educate the community and to educate physicians as well, because we know that’s how this epidemic arose in the first place,” Meier added. “It takes some coordination with public health departments and other community stakeholders.”
Meier said dopamine-boosting medications like methadone and buprenorphine can help to rewire a drug user’s brain after years of continued substance abuse. Other medications like naltrexone can negate the effects of heroin and other painkillers, essentially ruining the high for users who happen to relapse on the path to recovery.
The old guard, however, isn’t quick to change its ways. Meier said some “old school people” have actively opposed medication-assisted treatment under the false impression that it simply replaces one substance for another. He argued recovery rates are much higher with medication than standard, cold-turkey-style models.
“There’s just a lot of stigma surrounding treatment,” Meier added. “A lot of the work surrounding education and addressing misconceptions has been on the right track. The infrastructure for dealing with this, however, has been pretty thin. It’s great to have money but if you don’t have the providers to give treatment, it’s hard.”
Risper, publisher of the newspaper The New Citizens Press, said her neighborhood’s opposition is based entirely on striking a balance. She isn’t opposed to addiction treatment facilities; She just doesn’t want two to operate in her neighborhood. She once rented property to recovering addicts in the past, but “the whole thing was a mess” and led to a damaged doorway and costly repairs.
“We just need some balance. It’s too much,” Risper added. “This whole stigma thing is a crock of malarkey.”
Harris said one overdose is too many and he’s quickly growing tired of addiction preying on his community.
“We have to understand this is a community problem and it’s going to take the strength and the will of the entire community to come together and combat this,” he said. “It’s not going away on its own. It’s going to take time and education to turn the tide, and I think we as a community recognize this more than ever.”
Support City Pulse - Donate Today!
Comments
No comments on this item Please log in to comment by clicking here