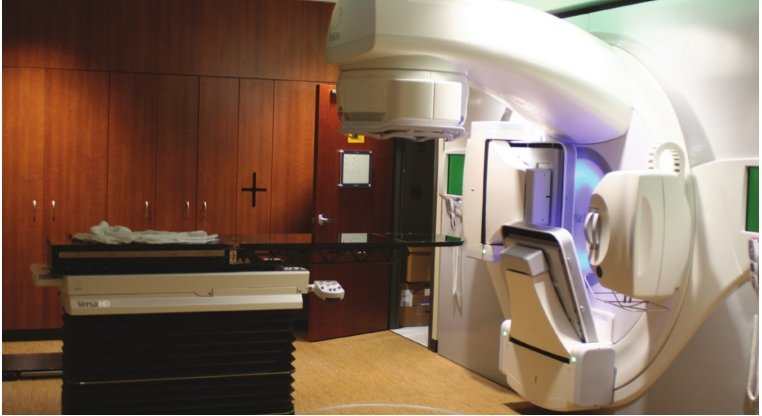
 Field notes from a revolution in cancer treatment
Field notes from a revolution in cancer treatmentAny cancer center, no matter how cutting edge its technology or cheerful its design, is a place where people get bad news.
But there’s more good news about cancer treatment than most people think, and the game is changing month by month.
Cancer treatment is swiftly moving toward individualized molecular and genetic tools that Sparrow Cancer Center’s director, James Herman, hopes will replace what he calls “MOAB” (Mother of All Bombs) forms of treatment such as radiation and chemotherapy.
Oncologist Tim McKenna, director of Sparrow’s breast clinic, has been in practice over 35 years. He said he more optimistic now than he has ever been.
“I can see where maybe breast cancer surgeons will be standing on street corners with cardboard signs,” McKenna said.
Already, many of McKenna’s patients never get a mastectomy or lumpectomy. Treatment that combines chemotherapy with monoclonal antibodies that target a patient’s particular cancer can get rid of a tumor without surgery in many cases.
McKenna said they take a couple of core samples “and say, ‘You know what? I guess there isn’t any cancer left. You’re done.’ I predict that in 15 years, 20 years, that will be 90 percent of the cure.”
Corrie Bourdon called it “a brave new world, amazing and life-saving.” As the cancer genetic counselor, a position created a year ago especially for her, Bourdon is Sparrow’s newest staff member and a herald of that new world.
“If you remember the ‘90s sci-fi movie, ‘Gattaca,’ it’s becoming real life,” Bourdon said.
Now, when cancer is detected, on cologists ask a whole new set of questions, using a strange new vocabulary. McKenna rattled off a few of the big ones: Is the cancer estrogen receptor positive? Does it overexpress her2/neu? What’s the Oncotype score? What’s the MammaPrint score?
To sample just one spoonful of that jargon stew, MammaPrint is a 70-gene map of the cancer itself, a genetic analysis that helps doctors decide if systemic treatment is warranted, even though they can’t prove the cancer might be somewhere else.
 “It allows us to predict recurrence down the road and take steps now,” McKenna said.
“It allows us to predict recurrence down the road and take steps now,” McKenna said.
Like the genetic engineers of “Gattaca,” Bourdon tests families for genes that predispose them to cancer. (People sometimes ask Bourdon if she designs babies. She tells them she doesn’t.)
If a person carries the mutation, the next step is extra screening or even preventative surgery to keep them from getting the cancer.
“The advances are exponentially increasing,” she said. “Cancer treatment and genetics are converging very, very quickly, if they are not already converged.”
Until recently, as Sparrow oncologist Joseph Meunier explained it, many chemotherapy drugs have been designed to treat a particular type of cancer, based on the part of the body affected, such as lung or breast cancer.
But recently, Meunier and his team have been successful doing things they never thought they would do, like treating ovarian cancer with skin cancer drugs.
They wouldn’t have thought of trying such a thing five years ago, because no body knew the two forms of cancer had the same genetic mutation in common.
“Just the leaps for ward in the last 18 months — it’s been absolutely unbelievable,” Meunier said.
A month ago, the FDA approved a chemotherapy type drug for the treatment of a genetic mutation, regardless of the organ of origin.
“That’s the first time that’s ever happened,” Meunier said. “I can’t even imagine, in the next 10 or 20 years, the way we look at therapy altogether is going to be entirely different.”
Genetically tailored treatment is not a silver bullet, though. Bourdon said the environment still plays “a huge role” in how people get cancer.
“Exposures to chemicals, pesticides, or they worked in a factory,” Bourdon said. “I’ve heard a lot about the Dow Chemical Plant in Michigan. Or if someone was in the military, who knows what they were exposed to?” But cancers have genes of their own that can be unlocked and, perhaps, manipulated to their distinct disadvantage.
“I would not be surprised at all if we actually have a cure for cancer in the next 10, 20 years, or we’ve at least made such advancements that you just go to your doctor and take a pill to fix your gene and you’re cured,” Bourdon said.
Gordan Srkalovic, oncologist and director of Sparrow’s clinical trials program, took a more circumspect view. Srkalovic has been an oncologist for 18 years and did basic oncology research before that. He has been at Sparrow 14 years.
“‘Are we going to conquer cancer?’ is a loaded question,” he said. “I don’t think we will be able to cure every patient with cancer, at least not in my lifetime.”
It’s more likely, Srkalovic said, that cancer will be cut down to size, from a “deadly, progressive disease” to a chronic one that can be treated, comparable to hypertension or high blood pressure, and that’s already happening.
“The goal at the present is to reduce the burden of disease to the point the patient could have cancer cells, but the cancer is controlled,” he said.
It’s a more modest prognosis, but still a dramatic leap from cancer outcomes a generation ago.
“When I started, you took a Magic Marker and you put an ‘X’ over where you thought the cancer was,” Herman said. “Then I’d pretend I’d know what was going on with the treatment.”
The cure rate for cancer has gone from 30 percent to 70 percent since Herman entered the field over 35 years ago.
“That means the cancer is gone and they die of something else,” he said. “You don’t hear about that 70 percent. They carry on and live their life. It’s a revolution.”
So McKenna may end up on a street corner with his cardboard sign after all. It seems perverse to dream of tearing down a building that’s brand new, but the Herbert-Herman Cancer Center is a special case.
“We love helping patients and curing them, but it would be amazing if we were all out of a job,” Bourdon said.
“I hope it is the last cancer center,” Meunier said. “I hope we don’t have to build a new one again.”
“Will we be able to get rid of buildings like this? I hope so,” Herman said. Herman is entitled to say that, with his name is on the place and all.
Support City Pulse - Donate Today!
Comments
No comments on this item Please log in to comment by clicking here